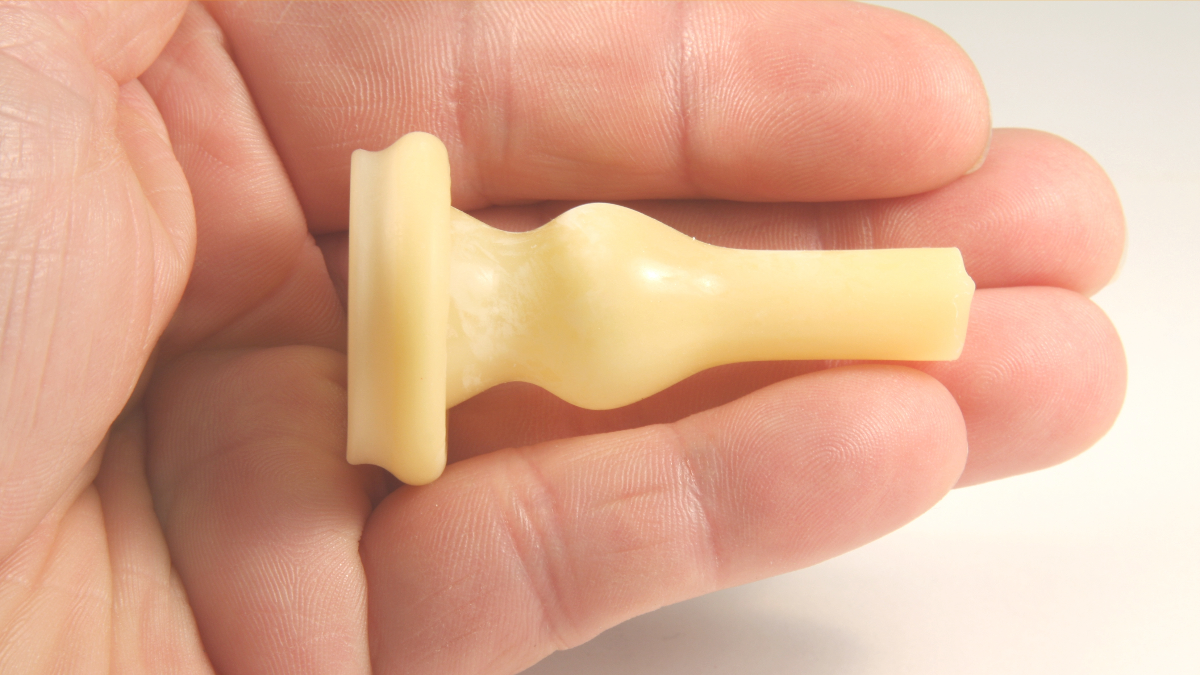
Men’s Liberty: Navigating the Learning Curve.
Simply put – the learning curve is a 2-3 day period needed for you to rid your skin of moisture to ensure the full adhesion time for Men’s Liberty. Your skin holds in moisture, naturally. In addition to the natural moisture content of your skin, the soap lotion or oils that you use daily can add more moisture to your skin. Men’s Liberty uses a proprietary adhesive called Hydrocolloid. A moist environment will lessen the adhesive qualities of the Hydrocolloid. During the first few days of wear-time, you may not have a full 24-hour wear-time from the Men’s Liberty due to the moisture content of your skin.
Read MoreSeven Uninspected Causes of Urinary Incontinence.
Urinary incontinence, a condition often associated with embarrassment and discomfort, affects millions of individuals worldwide, irrespective of age or gender. While common causes such as aging, childbirth, and certain medical conditions are widely recognized, there exists a realm of lesser-known factors that can contribute to this condition.
Read MoreNew Chapter: Uplifting New Year Resolutions for Older Adults
As the calendar turns and a new year beckons, it’s the perfect time for us to embrace fresh opportunities and set meaningful resolutions. In this newsletter, we’ll explore unique and uplifting resolutions tailored to enhance well-being, happiness, and fulfillment. Cultivate Lifelong Learning: Embrace the joy of learning by setting a resolution to explore new subjects…
Read MorePractical Tips on Tackling Incontinence Stains
Living with incontinence can be challenging, but dealing with the aftermath of accidents doesn’t have to be a daunting task. In this guide, we’ll explore effective ways to clean up incontinence stains and accidents, leaving no trace behind. Act Swiftly: The key to successful stain removal is to address the issue promptly. The longer a…
Read MoreNavigating the Holiday Season with Confidence: A Survival Guide for Individuals with Urinary Incontinence
The holiday season is a time for joy and celebration, but for individuals managing urinary incontinence, it can also bring unique challenges. In this comprehensive guide, we’ll explore practical tips and strategies to help you not only survive but thrive during the festive season. Preparation is Key: Plan by identifying accessible restroom locations at event…
Read MoreHidden Penis and Condom Catheters: Why They Aren’t Always a Compatible Solution
Condom catheters are commonly used medical devices for managing urinary incontinence in men. However, there are situations where they might not be suitable, and one such circumstance is when dealing with a hidden penis. In this article, we will discuss the challenges of using condom catheters on individuals with a hidden/buried penis diagnosis and why…
Read MoreOsteoporosis in Males: A Silent Health Threat
Osteoporosis is a bone disease commonly associated with older women, but it can also affect men. While it’s true that women are more susceptible to this condition, men are not immune to the risk of developing osteoporosis. In fact, osteoporosis in males often goes underdiagnosed and undertreated, making it a silent health threat. In this…
Read MoreMen’s Liberty™ and FreeDerm®
Together, Men’s Liberty and FreeDerm offer a comprehensive solution that not only provides reliable urinary control but also prioritizes patient comfort and skin health. Understanding Men’s Liberty Men’s Liberty is an innovative male external catheter designed to provide a reliable and discreet solution for managing urinary incontinence. Unlike traditional absorbent products like adult diapers, Men’s…
Read MoreBreaking the Silence: Understanding Male Breast Cancer
When we hear about breast cancer, our minds often jump to the image of women facing this challenging battle. However, it’s essential to remember that breast cancer doesn’t discriminate based on gender. While significantly less common, men can also develop breast cancer. In this blog, we’ll explore the lesser-known but crucial topic of male breast…
Read MoreCleaning Your Bedside Drain Bag
Recently, many of our wonderful Men’s Liberty patients reached out with questions about cleaning their bedside drain bags, and we’re here to help! We understand that cleaning your bedside drain bag is a crucial aspect of your urinary health maintenance and infection prevention routine, and we want to ensure it’s as simple as possible. Here…
Read More